Lymph Vein Lymph Graft
This method can be used in congenital lymphatic duct occlusion and segmental lymphatic duct occlusion. It had 75% efficacy among 133 patients with early stage secondary lymphedema and overall 50% efficacy in long-term follow-up.
Free lymphatic flap autotransplantation
Trevidic and Keolmeyer reported that transplanting the inferior axillary gland including latissimus dorsi and skin of the healthy side to the lesion had 75% efficacy.
Other techniques of microsurgery are being developed besides the ones mentioned above. Despite such advancement, microsurgery is rarely performed because it is a difficult procedure using 20X magnification, time-consuming (5-10 hours under general anesthesia), costly and few surgeons have expertise in the procedure. Microsurgery is becoming more popular in the US, however, at least 2-3 years of follow-up is needed to evaluate the outcome. Continuous compression therapy is needed after surgery.
[Advertisement] MAGNUM(Q-switched Nd:YAG Laser) – Manufacturer: (www.i-dana.com)]
Outcome of microsurgery
In a Western report, 1,214 patients with lymphedema were treated with microsurgery.
After surgery, the mean yearly volume reduction was .5-3.0cm in 149 stage 1 patients and 5-12cm in stage 2 patients.
Long-term follow-up of stage 1 and 2 patients showed that 40% of patients achieved normal volume, 28% experienced at least 50% reduction, 28% of patients experienced less than 50% reduction and 4% of patients had no change.
Overall, surgery was effective in 96% of patients. Inflammation was completely resolved in 68%, and reduced in 32%. Post-surgical lymphscintigraphy revealed new lymph circulation in 69%.
Two microsurgeries were carried out three months apart in stage 3 patients who experienced mean yearly reduction of 20cm with drastically reduced pain. Microsurgery is the most effective modality in patients unresponsive to combined physical therapy. Surgical outcome was better in the early phase of the disease and younger age of patients. It is important to carry out lymph drainage massage, compression stockings and bandaging for 1-2 months before and at least 6 months after surgery to obtain better results. Surgery is contraindicated in cases of inflammation or progressive cancer.
I would like to introduce the procedures offered at Yonsei S Hospital.
Yonsei S Hospital has been treating patients with lymphedema with various microsurgical procedures since 2008. Lymph node free graft brought clinical improvement but patient satisfaction was poor. Patients want rapid improvement but currently there are no treatment options in the world that can achieve that. As patients with lymphedema are aware that their chronic condition requires long-term treatment, they tend to research more about the disease and treatment. The following are some of the most common questions patients ask during consultation.
1. Isn’t surgery very painful? What kind of anesthesia is used?
2. Is surgery safe and are there serious complications?
3. Does surgery cause scarring or any other tissue damage? Does the condition recur?
4. Are the medical staff carrying out the surgery experienced and successful?
5. How many surgeries has the doctor performed?
6. Is the surgical outcome good? How soon can you see the improvement?
7. Does the doctor have a sufficient number of cases treated and photos?
8. Can the surgery be repeated?
9. What is the cost of surgery?
10. Do I have to keep wearing compression stockings and bandages?
At Yonsei S Hospital, we are committed to resolving such enquiries and continuously achieving a 90% satisfaction rate of patients. I post before and after photos on my blog so that patients and their caregivers can get a quick visual update. Moreover, based on a large number of cases treated, we provide a customized surgery technique for individual patients.
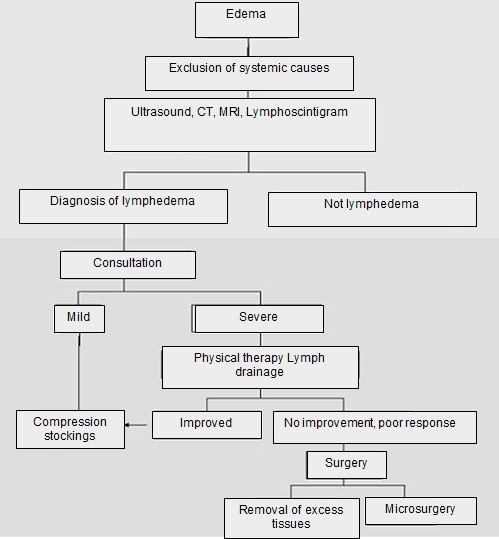
Image 1. Diagnosis and treatment process of lymphedema.
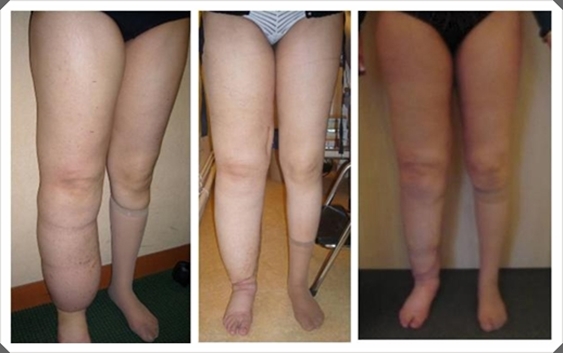
Image 2. Before and after (2 years) microsurgery.
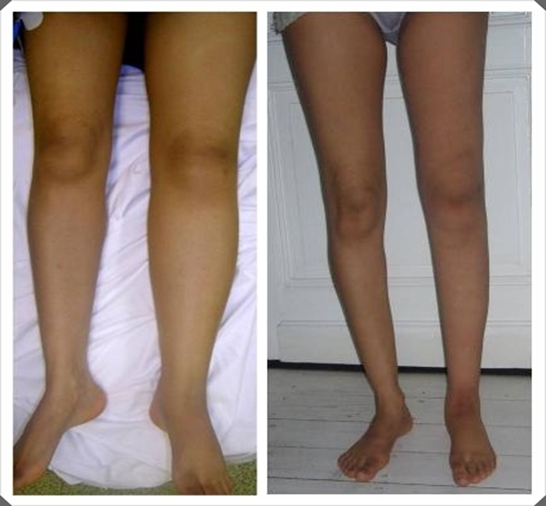
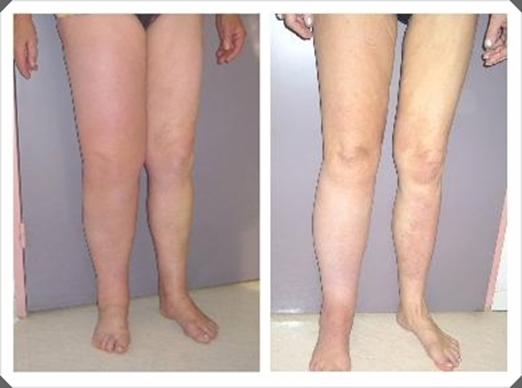
Image 3. Before and after microsurgery.
-To be continued-





















