Infection: Suspected cases and possible solutions
Infection is generally rare in dermatologic surgery (0.7~4.3%). Surgical infection develops from extrinsic or intrinsic intraoperative factors. Symptoms and signs develop 3-8 days after surgery. Symptoms and signs include pain, erythema, hot flush, edema, pus, cellulitis, lymphangitis, chills, fever, and adenopathy, etc. Surgical infection interferes with wound healing and increases the risk of wound dehiscence and skin necrosis as well as cause poor aesthetic outcome.
Staphylococcus is the most common causative microorganism. Infection occurs through the nose or perineum and manifests in cellulitis and abscess. Infection with Group A Beta-Hemolytic Streptococci (GABHS) develops symptoms quickly and can cause severe cellulitis and toxic shock syndrome within 24-48 hours. Pseudomonas aeruginosa infection occurs most often after ear surgery which can lead to chondritis and cellulitis.
Wounds are categorized as following to help predict risk of infection and determine the need for anaphylactic antibiotics.
Clean wound (Class I): 1~5% infection; aseptic surgery wound, cyst and tumor surgery wound without inflammation and contamination.
Clean-contaminated wound (Class II): 8~11% infection; a minor breakage of aseptic conditions. There is a contaminated area. Examples include oral or armpit surgery wounds, etc.
Contaminated wound (Class III ): 20~30% infection; the antiseptic condition is broken and there is a contaminated site. Examples include inflamed cyst and tumor wounds.
Dirty wound (Class IV) : 30~40% infection; the aseptic condition is broken and there is a contaminated site. Examples are traumatic or infected wounds.
Factors affecting infection include prolonged operation time, contact with foreign substance, compromised immunity, diabetes, liver or kidney failure, old age, traumatic shock on the wound area, excessive electrocauterization, excessive pulling of the wound, and wound contamination, etc. To prevent infection, aseptic techniques should be used. Below are steps needed for maintaining aseptic conditions.
Sterilization of the wound and hands: chlorhexidine (hibiclens), povidone-iodine (betadine), hexachlorophene (phisohex), benzalkonium chloride (onyclear), and isopropyl alcohol, etc. are used.
Use of sterilized equipment: Use sterilized and disinfected equipment. If the same equipment is used in one patient and immediately after in another patient, use high speed high pressure steam sterilization (sterilize for 10 minutes).
Disinfectant sterilization: high pressure steam sterilization, EO gas sterilization (for plastic etc. that cannot be steam sterilized).
A sterile gown, mask, gloves and cap must be worn.
[Advertisement] Ultra Skin/Pastelle – Manufacturer: WONTECH(www.wtlaser.com)
Criteria for using anaphylactic antibiotics are as following (Haas & Grekin, JAAD, 1995).
Indications
Some cases of clean-contaminated wound (Class II).
All contaminated wounds (Class III) and dirty wounds (Class IV).
Long operation time.
Weakened immunity.
Weakened general health.
Surgery of special areas such as the ear.
Usage: 1-2 hours before surgery every 24-48 hours. With confirmed infection, use for 7-10 days. Administer once, 1 hour before surgery. Post-surgery administration is carried out only in case of prolonged surgery or contaminated environment. Injection into the resected area can be considered. Apply topical antibiotics on wound closed before dressing.
Management of wound infection
Infection is suspected in wounds with pain, redness, swelling or discharge. Perform bacterial culture and susceptibility test. Check vital signs.
Wounds with abscess should be drained of pus. There is controversy over complete removal of sutures, however, sutures should be removed or resection is needed for facilitating drainage.
Completely remove sutures and cleanse the wound twice a day and apply dressing. Use topical antibiotics, chlorhexidine cleansing, iodoform gauze wet dressing, and wet-to-dry dressings, etc.
Perform blood culture in case of high fever and take additional measures.
Use below empirical antibiotics against suspected bacteria before culture results are produced. After obtaining results, use appropriate antibiotics for confirmed strain. Switch to appropriate antibiotics according to clinical symptoms, disease progression, and complications, etc.
S.aureus and GABHS: 1st generation Cephalosporin, Quinolone, Erythromycin, Clindamycin.
Gram negative bacteria: 1st generation Cephalosproin, TMP/SMX, Quinolone.
Pseudomonas (ear infection): Quinolone.
Wound infection should be confirmed after considering the following symptoms and signs.
Allergic contact dermatitis, irritant contact dermatitis.
Suture reaction.
Inflammatory reaction after surgery properly carried out.
Hematoma, seroma.
Tissue slough (skin tissues yellowed from partial necrosis, Image 2).
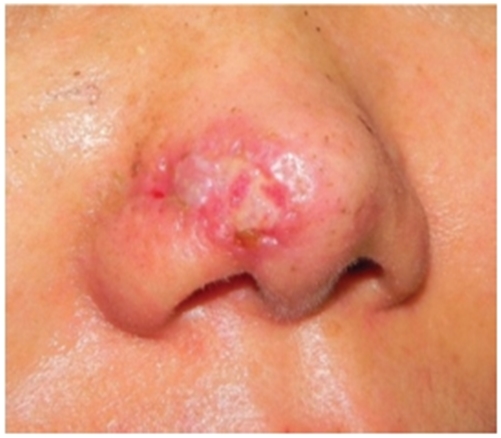
Image 2. F/43. Slough developing from partial necrosis of the flap after pigmented basal cell carcinoma surgery.
-To be continued-





















