6. Dehiscence
1) Risk factors of dehiscence are described below. Being familiar with them would help prevent dehiscence.
A. When no subcutaneous suture thread was used.
B. Risk factors.
① Old age
② Nutrition
③ Underlying conditions such as diabetes
④ Environmental stressors
⑤ Medication
⑥ Suture-related factors: Infection, hematoma, seroma, tension on the wound, excessively early removal of suture, accidental trauma
2) Once dehiscence occurs, the following measures can be taken.
A. If there is no infection.
① Occurring within 24 hours – Resuture
② Occurring within 24-48 hours – Clean and resuture
③ Occurring after over 48 hours – Secondary wound closing, Address the cause (infection, hematoma, and necrosis, etc.)
④ If the wound is clean sterile strip may be better than resuture. (Reference 3)
B. Patient education: Consider secondary wound closing in cases with limited post-surgery excercise, and muscle use (lifting heavy objects), etc.
C. For, wound dehiscence with inflammation and crust (Image 3, B), debride the necrotic tissues and perform secondary wound closing with silver dressing.
3) Following areas are susceptible to wound dehiscence.
-Joint areas-neck, knee, elbow, deltoids
-Areas bearing the body weight-foot, lower limbs
-Compressed areas-hips
- Facial areas with high sebum production
[Advertisement] A-One LITE(Facial Diagnosys System) – Manufacturer: BOMTECH(www.bomtech.net)
4) Following should be considered in cases of dehiscence.
-It is mostly associated with buried materials (suture, collagen foams, etc.) and occurs in a few weeks to a month after surgery.
- It can be treated with injection of Triamcinolone(10mg/ml) into the lesion with or without removal of foreign body.
- Consider removal of the wound or foreign body if possible.
- Consider using suture materials different from the initial suture.
- Hemorrhagic granuloma can occur with the use of anticoagulants.
- Consider incision, drainage and antibiotic therapy if the patient has coagulopathy.
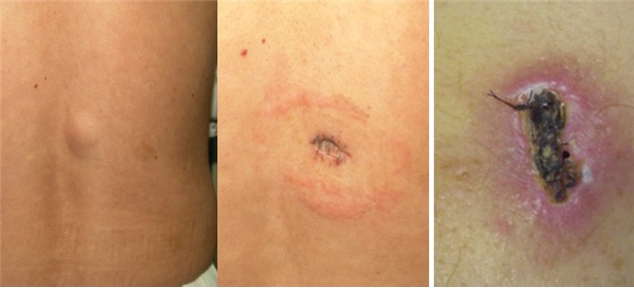
Image 2. Wound dehiscence after lipoma removal (A), Wound with infection and crust (B).
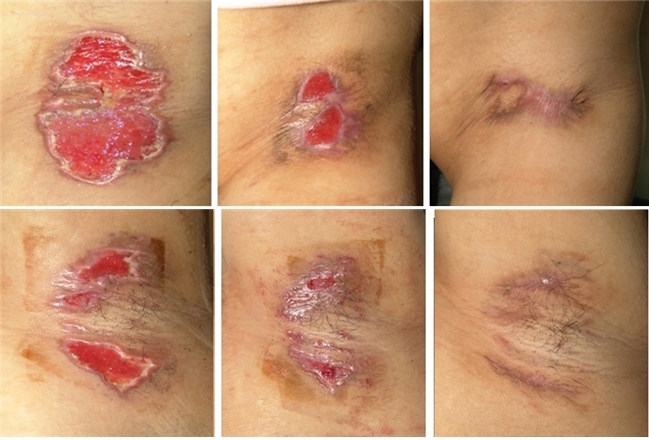
Image 3. PIH and partial hypertrophic scar occurred after secondary wound healing of the skin necrosis following subcutaneous laser coagulation of both armpits.
-To be continued-





















